Improve Your HEDIS and Star Ratings by Closing Patient Care Gaps

HEDIS and Star ratings play an important role in ensuring the success of healthcare organizations as both businesses and purveyors of excellent patient care. In this blog, we will cover the basics of HEDIS and Star ratings and end with ways to improve your scores by closing care gaps.
What is HEDIS?
The Healthcare Effectiveness Data and Information Set (HEDIS) is a set of performance measures used to assess the effectiveness of health insurance plans. The measures set goals for care across a range of health issues, with a focus on preventative care.
It was created by the NCQA as a tool to ensure that healthcare delivery systems were adequately serving patients. HEDIS scores give health plans a snapshot of how they are performing and ways they can improve the delivery of certain services.
What are Star Ratings?
Star Ratings is a similar tool that measures health plan effectiveness. Unlike HEDIS, which measures all healthcare plans, Star Ratings are applicable to Medicare Advantage plans and Medicare Part D Prescription Drug plans.

What is the Difference Between HEDIS and Stars?
Many people have questions about HEDIS vs Stars and what they each mean. In practice, the goals of the systems are almost identical. Both rating systems assess care delivery with the goal of encouraging health plans to improve access to care and the patient experience.
The two rating systems apply to different types of health plans. In addition, they are not operated by the same agency. HEDIS is managed and defined by the National Committee for Quality Assurance (NCQA), which collects performance data via an annual survey. Star ratings, on the other hand, are managed by the Centers for Medicare and Medicaid Services (CMS). CMS collects data using a variety of surveys to facilities, providers, and patients and uses the data to score health plans.
HEDIS and Diabetes
Due to the increasing prevalence of diabetes, diabetes care is a priority area under HEDIS. NCQA has developed a comprehensive set of HEDIS measures related to care for diabetic patients. The measurements include a list of the essential medical care that should be included in a comprehensive diabetes care plan.

Those measures consist of:
- Hemoglobin A1c testing (HbA1c poor control >9, HbA1c control <8)
- Blood pressure control (<140/90 mmHg)
- Eye exam (retinal) performed
- Medical attention for nephropathy
All of the measures in the diabetes care area are focused on preventative care and care that improves outcomes for individuals with diabetes. The screening exams all address health risks associated with diabetes. The information provided from these screenings allows doctors and patients to adjust treatment plans as needed.
Retinal exams are integral for diagnosing and managing a serious eye condition called diabetic retinopathy. In the past, these exams required a trip to an eye doctor, and not all patients could get these exams regularly, leading to gaps in basic diabetes care. Increasing access to proper eye care is essential for in-home care providers performing health risk assessments to close the existing gaps in comprehensive diabetes care.

Investment in new technologies, such as tools for retinal screenings, can make it easier for in-home care providers to offer preventative diabetic exams to a greater number of patients.
How Access to Retinal Exams Can Improve HEDIS Ratings
Anyone with diabetes is at risk of diabetic retinopathy, and the risk increases with every year that an individual has diabetes. Diabetic retinopathy is one of the leading causes of vision loss and blindness in the United States. Early detection of the condition can be simple and cost-effective and can be done with non-invasive retinal screenings. These tests allow individuals and their healthcare providers to take steps to slow the progression of the condition.

Source: Centers for Disease Control (CDC.gov)
Eye exams are considered performance measures for diabetic care under both HEDIS and Star rating systems because they can improve outcomes for diabetic retinopathy. Improving access to retinal screenings can increase the number of patients who receive these exams. As a result, providers and payors can report those increases and improve their ratings for diabetic care.
Early Detection Reduces Risk of Preventable Blindness
Diabetic retinopathy is an eye disease caused by high blood sugar levels, which damage blood vessels in the retina. These blood vessels can swell and leak or become obstructed, preventing blood flow within the retina. If the condition progresses, the damage can lead to vision changes or blindness.

When diabetic retinopathy is detected early, individuals can slow the progression of the condition by controlling their blood sugar and managing their overall health. If diabetic retinopathy progresses to more advanced stages, treatment is more complex. Treatment may require medication or surgery, and vision changes caused by advanced diabetic retinopathy cannot be reversed.
Screening exams facilitate early detection and management of diabetic retinopathy. In addition, they provide an entry point for valuable discussion between patients and providers about diabetes management. Patient education can provide individuals with the tools they need to lower their risk of preventable blindness and effectively manage diabetes in the long term.
Why HEDIS and Star Ratings Matter
HEDIS and Star ratings are publicly accessible demonstrations of the efficacy of patient care and preventative healthcare practices. Consumers can use HEDIS scores and Star ratings to help them decide on healthcare providers or insurers, informing their choices about the care delivery systems they eventually choose.
Low HEDIS or Star ratings indicate that a certain plan has gaps in care. This, in turn, may reduce confidence in the services an organization offers. By increasing access to preventive care screenings and closing those patient care gaps, you can improve your HEDIS score.

HEDIS and CMS Star ratings can also affect funding levels for healthcare organizations and insurance payors. If an organization has high Star ratings or HEDIS ratings, it could see a boost in funding. Conversely, an organization with low ratings could struggle to qualify for reimbursement and see financial penalties.
To give an idea of how much an organization has to gain from a high HEDIS or CMS Star rating, a health plan with 100,000 members would qualify for $17 million in reimbursement for each quality measure taken. Organizations with less than four stars do not qualify for bonus payments. In addition, low ratings can negatively affect contracts or partnerships with third-party entities that work with payors or providers.
So, what’s the best way to ensure HEDIS gap closure and boost HEDIS and CMS Star ratings?
How In-Home Care Providers are Improving NCQA HEDIS and CMS Star Ratings with IRIS
To close gaps in care, HEDIS-based organizations can implement new ways to deliver care to patients who might not otherwise have access to it. Many providers are starting to administer preventative screenings through in-home evaluation health visits and screening events to increase the number of patients receiving preventative care.
Employing innovative ways of delivering care to patients outside the clinic environment closes care gaps and benefits everyone in the healthcare delivery system. Patients benefit because they get the screenings they need in a convenient manner. Providers benefit because their HEDIS ratings go up with every additional screening performed. Insurers benefit because the chances of catching the development of a more serious condition are higher.
The IRIS solution helps HRAs, in-home health organizations, and other healthcare systems close gaps in access to diabetic retinopathy screening to reduce the risk of preventable blindness. The solution can be deployed in multiple environments, such as home care, residential facilities, screening events, community-based clinics, and primary care offices. This allows for the performance of retinal screenings without the need for a separate ophthalmology appointment.
The technology is easy to use and compatible with a variety of handheld and tabletop fundus cameras. IRIS-trained HRA employees can use the system to capture a patient’s fundus image. The image can be instantly sent through the cloud to our secure servers. It’s enhanced by our algorithm and delivered to the IRIS Reading Center (IRC), where the image is interpreted by one of the IRC’s physicians. The results are then available to the appropriate healthcare providers and the patient.
Improve Your Preventative Screenings with IRIS Today
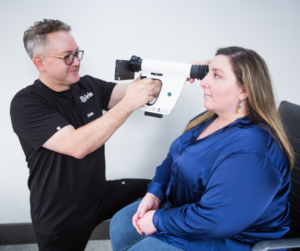
For years, IRIS has been working with in-home health evaluation organizations, HRAs, and healthcare providers (HCPs) to address HEDIS care gaps and improve HEDIS and STAR measures by making it easier for patients to receive eyesight-saving examinations. Our image-enhancing technology, paired with portable fundus cameras, makes diabetic HEDIS measures easier to meet by helping providers meet diabetic patients wherever they are in their health journey.
Our solution is used by organizations such as Prisma Health, St. Elizabeth’s Healthcare, and Gateway Medical. You can check out more of our client’s success stories here, or if you’re interested in trying IRIS yourself to close HEDIS gaps and improve CMS Star ratings, you can reach out to us today to schedule a demo.
Frequently Asked Questions
What is the star rating?
Star Ratings are methods of evaluating and distributing information related to Medicare Parts C and D health plan quality and performance. They provide insights into how well the health plans are currently performing in terms of adherence to established quality measures.
What are HEDIS measures?
The Healthcare Effectiveness Data and Information Set (HEDIS) is a set of standardized performance measures applied to healthcare providers, facilities, and health insurance plans on important dimensions of care and services.
What is a HEDIS score?
NCQA conducts surveys of health plans and Preferred Provider Organizations (PPOs) using the Healthcare Organization Questionnaire. In addition, NCQA collects non-survey data via the Interactive Data Submission System. NCQA assesses the data to determine how well plans are meeting HEDIS measures and assigns a score based on the results.
What are the main categories of Star rating measures?
Star Ratings measure plans across five categories:
- Health outcomes: Measures of improvements to a beneficiary’s health based on the care provided
- Intermediate outcomes: Measures that contribute to health outcome measures
- Patient experience: Measures of beneficiaries’ opinions about the care they’ve received
- Access to care: Measures of issues that may result in barriers to receiving care
- Process measures: Capture the ways health care is provided
How are CMS star ratings calculated?
Star Ratings are based on performance measures and surveys, including the CMS Health Outcomes Survey (HOS) and The Medicare Advantage and Prescription Drug Plan Consumer Assessment of Healthcare Providers and Systems (MA and PDP CAHPS). The performance measures are developed by the National Committee for Quality Assurance (NCQA), Healthcare Effectiveness Data and Information Set (HEDIS), and the Pharmacy Quality Alliance (PQA).
How to improve Medicare star ratings?
Healthcare providers and health insurance plans can improve their star ratings by enhancing their performance on key measures. Increasing access to care and ensuring more patients receive high-priority preventive screenings is one strategy for increasing star ratings.
SM 132, Rev C
Get started with IRIS today.
Want to know if IRIS is right for you? Schedule a one-on-one consultation with our team. We’re here to help.